Minimizing the risk of lab animal allergy (LAA) is an increasingly important design and operational consideration in animal research facilities, since LAA has been identified as one of the most significant occupational health risks for personnel working with laboratory animals and in the lab animal environment. Personnel exposure to allergens can be effectively reduced with facility design and engineering controls, including differential air pressures, directional air flow, HEPA filtration, automation, traffic patterns, separation of personnel space from animal space, as well as optimal use of personal protection equipment (PPE).
“Formal health and safety advice for LAA now exists in the United States and the European Union, since it is widely recognized as a health concern,” says Timothy Mandrell, DVM, DACLAM, vivarium planning/research animal program consultant for TDM Consultants in Memphis, Tenn. Mandrell is currently interim director of veterinary resources at the University of Maryland, Baltimore, and serves on accreditation teams for the American Association for Accreditation of Laboratory Animal Care (AALAC).
“LAA is something I deal with on a daily basis as a lab animal veterinarian and consultant, but it can be overlooked during the design and engineering phase of projects,” cautions Mandrell.
LAA occurs when an individual has an immune response to animal allergens found in urine, fur, saliva, or serum of laboratory animals. Symptoms of LAA are similar to other allergies, including nasal congestion, sneezing, itchy eyes, rashes where animals come into contact with the skin, or asthma, and in severe cases, anaphylaxis. Contact can occur through inhalation of particles in the air, direct contact with eyes or skin, or percutaneous exposure such as bites, scratches, needle sticks, or exposure through open wounds.
Mandrell points to five engineering controls that can reduce or eliminate exposure to allergens in animal facilities:
- Ensuring proper directional airflow and differential pressures
- Utilizing devices that capture and contain airborne allergens
- Using automation to reduce personnel exposure
- Separating personnel space from animal program space
- Optimizing workflow to avoid cross-contamination
Capturing and Containing Airborne Allergens
The Guide for the Care and Use of Laboratory Animals recommends 10 to 15 air changes per hour in animal holding facilities. The Guide also states that spaces containing hazards should have negative air pressure differentials with respect to surrounding areas. According to Mandrell, directional airflow should be negative to rooms with allergens, including animal hold rooms, procedure rooms, specialized animal research equipment rooms, and areas containing soiled cage washing equipment.
Proper equipment should be installed in the animal areas to capture and contain allergens, because it is highly effective at reducing personnel exposure to laboratory animal allergens. The most commonly used devices are:
- Ventilated Caging – Pressure can be positive when more air is going into the cage and differential pressure is positive inside the cage compared to the room, or negative when more air is taken out of the cage and the differential pressure is negative inside the cage. The latter is used when dealing with potentially pathogenic agents such as ABSL-2 or ABSL-3.
- Biological Safety Cabinets are considered the gold standard for allergen protection, since anything that is volatized inside the cabinet is captured by a HEPA filter. This type of cabinet meets certified safety standards set by the National Sanitation Foundation (NSF). To provide the highest level of protection for personnel involved in changing soiled cages, animal cage changes can be done within biological safety cabinets.
- Animal Change Stations – Used alone, this equipment does not meet NSF standards and should not be used with known biological hazards. However, animal change stations are still an effective engineering control to capture allergens and keep animals clean during handling.
- Workstations with Downdraft are used most often for animal procedures or surgical settings where a full cabinet is not possible. The downdraft units create a negative pressure at the surface with allergens captured by directional airflow.
“Automation is being used more and more in animal settings since it is a very effective way to protect personnel from harmful allergens and avoid cross-contamination,” says Mandrell. “Robotic arms can safely complete potentially dangerous and repetitive tasks, such as dumping soiled cages and cage washing.”
Separating Personnel Spaces from Animal Spaces
“Ideally office administrative areas should be separated from animal program areas to minimize the risk of allergens in administrative areas where personnel are not protected by PPE. It is surprising how many facilities try to combine both of these areas to save space without considering the health effects to workers,” says Mandrell.
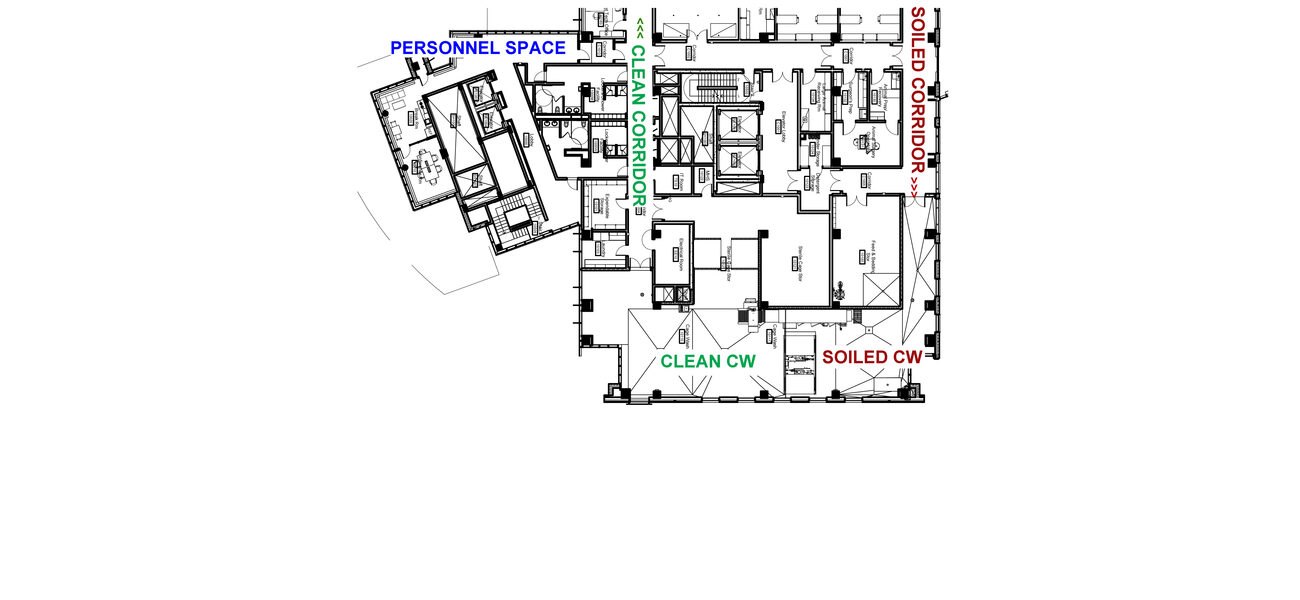
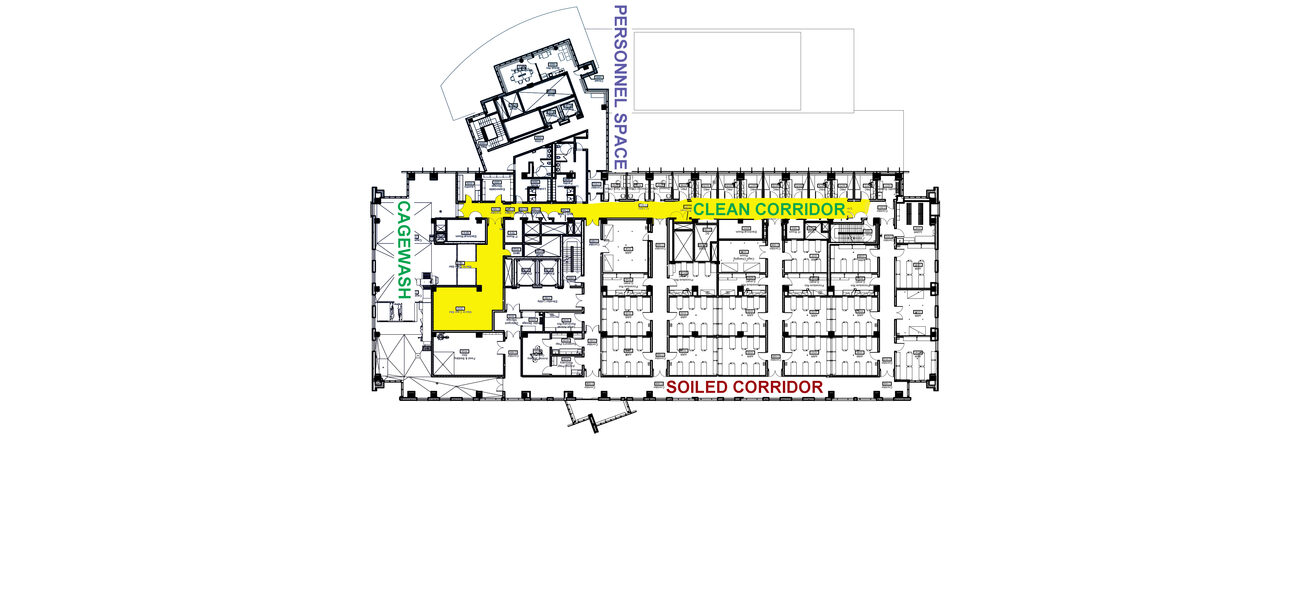
Mandrell explains that even when animal facilities separate administrative offices from the animal areas, spaces such as locker rooms and break rooms should also be considered to ensure that those spaces are pressure-positive to any corridor that is adjacent to animal procedure or holding spaces. He points to the Health Sciences Research Facility III at the University of Maryland, Baltimore, as a good example of a facility that effectively separates personnel space from high-risk animal space: Personnel space is located off of the clean corridor and clean cagewash area, physically isolated from the animal space. This provides a separation from the potentially harmful animal procedure rooms and animal support space located near the soiled cagewash and soiled corridor.
“University of Maryland has the luxury of space in this particular building, giving them the ability to avoid cross-contamination with a flow that keeps the soiled corridor completely separate from the clean corridor with a very defined path,” says Mandrell.
“When architects start looking for ways to save square footage, entries and exits are always easy targets,” says Mandrell. “However, facilities with animal research should maintain enough square footage in entries and exits to allow personnel to use PPE in the correct way.”
Mandrell concludes that optimal facility design includes entry and exit areas that allow for the best PPE practices, including designated space for donning and doffing PPE, an entry vestibule or interlock, PPE and handwashing stations, and receptacles for soiled PPE.
Below are links to key industry documents addressing lab animal allergies:
- Preventing Asthma in Animal Handlers published by the National Institute of Occupational Safety and Health (NIOSH)
- Guide for the Care and Use of Laboratory Animals published by the Institute of Laboratory Animal Research (ILAR), National Research Council
- Occupational Health and Safety in the Care and Use of Research Animals published by the Institute of Laboratory Animal Research (ILAR), National Research Council
By Amy Cammell