Health education institutions nationwide are pivoting toward instructional programs anchored around interprofessional team-based care models that satisfy accreditation requirements and better prepare tomorrow’s healthcare professionals by simulating real-world environments. In addition to improving outcomes, integrating multiple departments with shared resources can also increase space efficiency and lower operating costs. But these types of collaborative, interprofessional education facilities also include flexible labs, advanced simulation spaces, large team-based classrooms, and informal learning spaces that can lead to larger footprints and higher buildout costs, which means they need to be well considered and planned. Additionally, the cultural and pedagogical changes required by faculty can meet with resistance, as the boundaries that traditionally defined separate departments dissolve.
New interprofessional education facilities, such as the recently completed College of Health and Behavioral Studies (CHBS) building at James Madison University, provide valuable insight into overcoming cultural challenges and align building design with modern team-based healthcare curriculums. The multi-disciplinary CHBS facility was built as part of an initiative to combine different departments from disparate locations across campus that previously didn’t interact closely.
“We wanted to bring these departments together and collocate them for interprofessional education, so they could feed off each other and work together,” says Sharon Lovell, dean of CHBS. “But those departments were also used to having their own spaces. They each had their own identities and were used to functioning independently. That can be a real barrier to teamwork and collaboration. There’s always a natural resistance to change that needs to be resolved if you want to create buildings with programs that are effective for students.”
The new CHBS facility is organized so that no department dominates any one floor. Instead, department-branded learning spaces are strategically distributed throughout the building, allowing each department to maintain its unique identity while promoting cross-discipline collaboration.
“The goal of interprofessional education is to get students together in new ways of teaming. That involves a different form of education than faculty are typically used to at institutions of higher education. Collaborative planning, joint decision-making, and forging a common sense of purpose are critical to success,” says Lovell.
Shared resources include mannequin and standardized patient labs, a health assessment lab, and an advanced dietetics suite with a food prep and nutrition analysis lab. The building also houses occupational therapy and athletic training spaces, group therapy rooms, and a home environment lab. A year after opening, the diverse space programming and shared resources are already resulting in an increase of cross-program grant work and collaborative innovation among departments.
New Visioning + Positive Disruption
Managing cultural and programmatic changes within an organization requires sensitivity to the perceptions and expectations of all the stakeholders throughout the process.
“Different disciplines have different ways of thinking about what is important in the education of their students, and what kind of technology is important. It’s also very likely that there will be faculty who imagine the next generation of the kind of space they currently have. They need some help visioning what education will look like in 10 or 20 years, not just the next few, because the life of a building is long enough that you need to be visionary and think creatively,” says Lovell.
Change management strategies that worked for the CHBS included formation of an academic leadership team whose members could proactively work with faculty and campus partners to communicate the goals and intentions of the facility, while keeping them updated on progress throughout the process.
“To overcome these challenges, you really have to disrupt what people are used to. You have to disrupt the culture, the processes, and in some cases the curriculum. But that can lead to very innovative solutions that are forward-thinking and set the stage for training far into the future,” says Lovell.
Since the college was founded at the same time strategic planning for the new building began, there was an opportunity to redefine how the health science and behavioral studies disciplines would operate within the facility prior to construction. This allowed ample time for faculty participation in the planning process and the ability to align pedagogical goals with space design for a strongly unified outcome.
“As part of the process, I invented a term I call ‘new visioning,’ because I felt that what we were doing before was basically revisioning existing education spaces. This is really about creating a new vision that supports what tomorrow’s students need and sets the stage for training far into the future,” says Lovell.
Interprofessional Spaces
James Madison University’s health science and behavioral studies disciplines were joined together with other healthcare disciplines to create the new interprofessional college. As a result, simulation spaces were designed to be highly flexible and easy to reconfigure for different disciplines and scenarios.
“We are frequently changing simulation scenarios. We may have a hospice set up in one of our hospital simulation rooms for a week. Then we may need to set it up for a family simulation the next week—where a mother and child have been in an accident, for example—so, they would need to be in adjoining rooms. We can pull everything out of our simulation spaces and make a completely different type of room very quickly,” says Lovell.
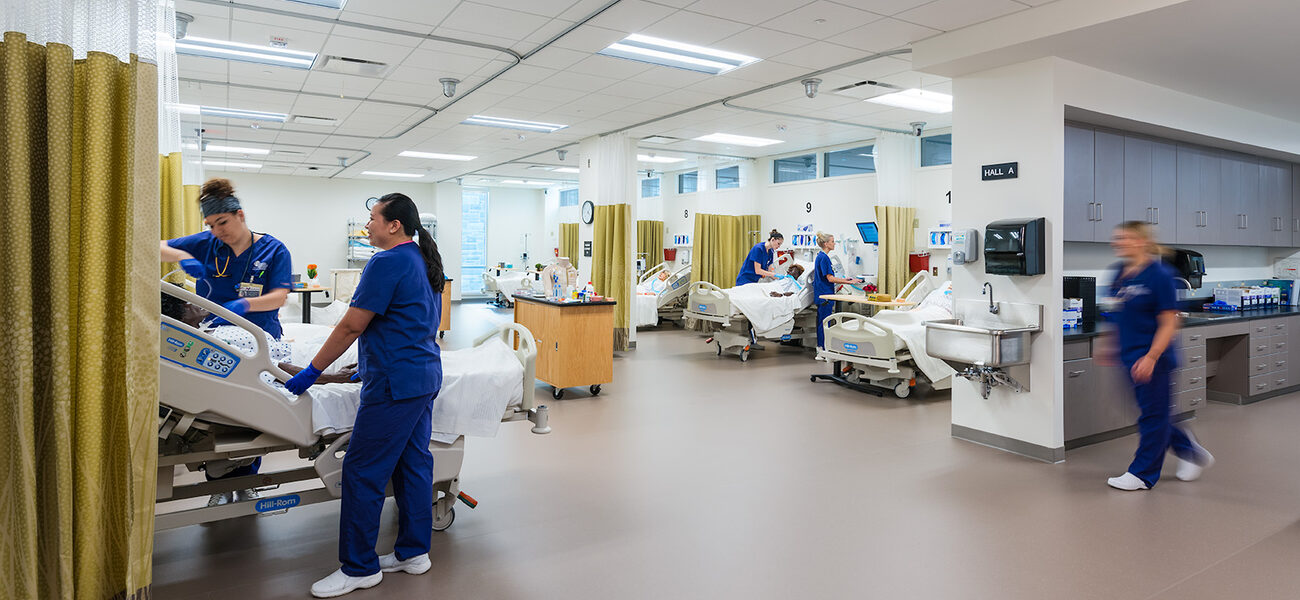
Likewise, teaching labs in the facility are used by both physician assistant and nursing programs in order to maximize shared resources. These spaces are designed so they can be subdivided by application, allowing both programs to use different areas at the same time. They are also large enough for multiple students to gather around the clinic beds.
“Students need to have experiences very early in their academic programs where they are interacting with actors, patients, clients, and each other in collaborative team-based environments,” says Lovell.
The building’s team spaces are designed so that the furniture can be arranged conference style or split up into small workgroups. Tables can be moved and assembled for various applications. Multiple monitors allow for easy sharing of information and communication.
“We’ve already seen significant payoff in the form of a very large grant coming to us because we focused on innovation and how we can share technology throughout the building,” says Lovell.
Previously, faculty didn’t have the kind of flex space that easily could be adapted to research or proposal writing. There were no convenient surfaces where you could set equipment, and the technology was not as robust. In the new facility, innovation labs provide large, flexible, high-profile spaces for collaboration, and the dietetics food lab has multiple identical work stations where students can explore how foods change when they’re manipulated or combined.
“In this kind of science, you need to be able to see and taste things. Now we have technology that allows for the instructor and students to watch what is happening in real time with the capability for immediate interaction and learning. This allows us to teach food science in ways that we weren’t able to in the past,” says Lovell.
Metrics + Expectations
EYP Architecture & Engineering, which has designed multiple interprofessional educational health facilities, including the CHBS, has identified a series of trends occurring across many of their projects.
“We’ve designed five projects recently that are all very similar in size,” says Jennifer Amster, a health education planner with EYP. “They all were trying to accommodate a changing pedagogy, and they all had the same goal of bringing together disparate groups to provide interprofessional opportunities in the new facility.”
From a design perspective, the big questions are: What things make a building uniquely interprofessional? And how do you create spaces that support the educational component, the community component, and the simulation component required in these types of facilities?
“The theme we keep hearing in these projects is the desire for a resource-rich environment. Because multiple groups are going to be using it, and they don’t know exactly how they’re going to be used yet,” says Amster.
Interprofessional education facilities typically include classrooms, informal spaces, simulation spaces, and collaborative team spaces.
“Configuration of the team-based learning space is where we have the most conversation in interprofessional facilities. We really want to look at the type of curriculum, the proportion of lecture to team-based activities, the types of technology to accommodate, and the size of the teams and utilization. Ultimately, we want to help define the frequency and types of change needed in the rooms, because there is a cost associated with varying types of flexibility, such as access flooring, moveable partitions and column-free large spaces,” says Amster.
Simulation spaces vary greatly depending on the unique needs and culture of the school. While traditional bed stations for three to four students in skills labs are typically 8 by 8 feet, the University of Texas Medical Branch (UTMB) wanted to have up to 10 learners around a bed at a time in their new shared Health Education Center, so their stations are 10 by 13 feet.
“That can start to add up and have an impact. But you need that much space for 10 learners, because now you’re bringing in a whole different team. It’s a big traditional break,” says Amster.
“When you are doing interprofessional education, you have to account for the number of people who are going to be around the bedside,” says Elissa Kellett, architect with EYP. “Even though we do these buildings thinking there is an economy of scale, when you bring this many professions together to serve a patient, you need more space than you would otherwise.”
Simulation space at UTMB averages 200 sf per hospital bed. In contrast, NYU Rory Meyers College of Nursing—which wants a maximum of four learners around the bed—allocates only 142 sf per bed. In the CHBS, the average is 170 sf per bed. Another issue is the amount of storage space required to support these kinds of flexible simulation spaces.
“We’ve started doing metrics for our own projects, and we’re seeing that you need an additional 0.3 sf for every 1 sf of simulation space, or another 30 percent,” says Amster.
Another difference is that these types of facilities also require larger classroom spaces.
“We use 30 sf per seat all day long for large flexible classrooms, but what we’re really finding, particularly with smaller teams at the tables, is that you need more like 35 to 40 sf per seat,” says Amster. “This allows for adequate acoustical separation and instructor circulation between the tables. That is a big ‘a-ha’ moment for people who are reviewing the project in terms of efficiency, because it makes for a super-big room. That means it no longer meets many states’ guidelines for a traditional classroom, which could be as low as 22 sf per student. We refer to these spaces differently in our program definition as a teaching lab or a learning studio.”
“For health education, particularly on a graduate level, you want to look at some of the latest undergraduate facilities too, because that’s where your students are coming from and what they are used to,” says Kellett.
By Johnathon Allen