A two-year, $55 million renovation at the University of Illinois at Urbana-Champaign’s Everitt Laboratory has transformed the four-story, 136,763-sf building into the first engineering-based medical school in the country, with a focus on medical simulation, research, and instruction. With final completion in June 2018 and the first medical classes starting in July, the Carle Illinois Medical School’s state-of-the-art features enable bioengineering students and future medical professionals to engage in project/problem-based learning and maximize their medical training by using the latest simulation and virtual reality technology.
“We’re changing the way we look at medicine with a curriculum that has projects based on open-ended questions,” says Liang Liu, PhD, associate dean of facilities and capital planning at UIUC’s College of Engineering. “We wanted an environment that supports open collaboration and encourages team building. The next generation of doctors—of healthcare providers—will be a lot more innovative and inventive.”
Built in 1949, the facility previously housed the Electrical and Computer Engineering Department and now accommodates the Bioengineering Department and medical school. The new class of 32 engineering-based medical students will soon complete the first of four years with fully paid tuition.
Realistic Medical Environment
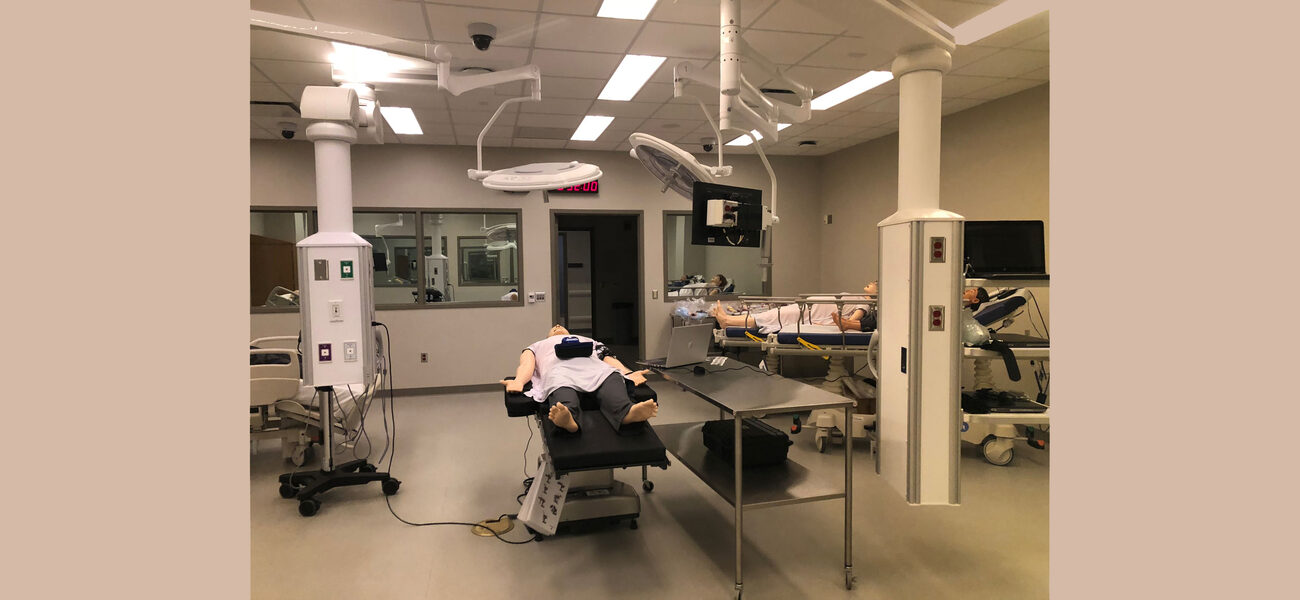
On the ground floor is the heart of the facility—the JUMP Simulation Center—where students use their surroundings and equipment to better understand and practice medical procedures prior to working on real patients. The center has an operating room, intensive care unit, and clinic exam rooms.
“We have to be 100 percent simulating what is out there in the real world,” says Greg Larson, director emeritus in the UIUC Office for Facilities Management, College of Engineering. “The environment has to be sterile. You know when you go to the doctor and they have all the medical walls with things like oxygen? We have both moveable and fixed versions of that equipment.”
The building also includes real, integrated diagnostic equipment and surgical lighting for the clinical areas and surgical suite. Cameras are installed throughout, says Larson, to comply with Health Insurance Portability and Accountability Act (HIPAA) requirements, as well as for accreditation. Students may have a case study that requires them to stop the bleeding on a mannequin or assess a potential heart attack, for example. They are then monitored for response times and accuracy, all within an environment of realistic sound effects and visuals.
They are capturing data to be able to critique medical students after they’ve performed a surgery, or interacted with patients, explains Larson.
The medical simulation center presents real-time opportunities to students, who can develop a product or device in a research lab and then immediately test it on the mannequins used in surgical suites.
Learning with Technology
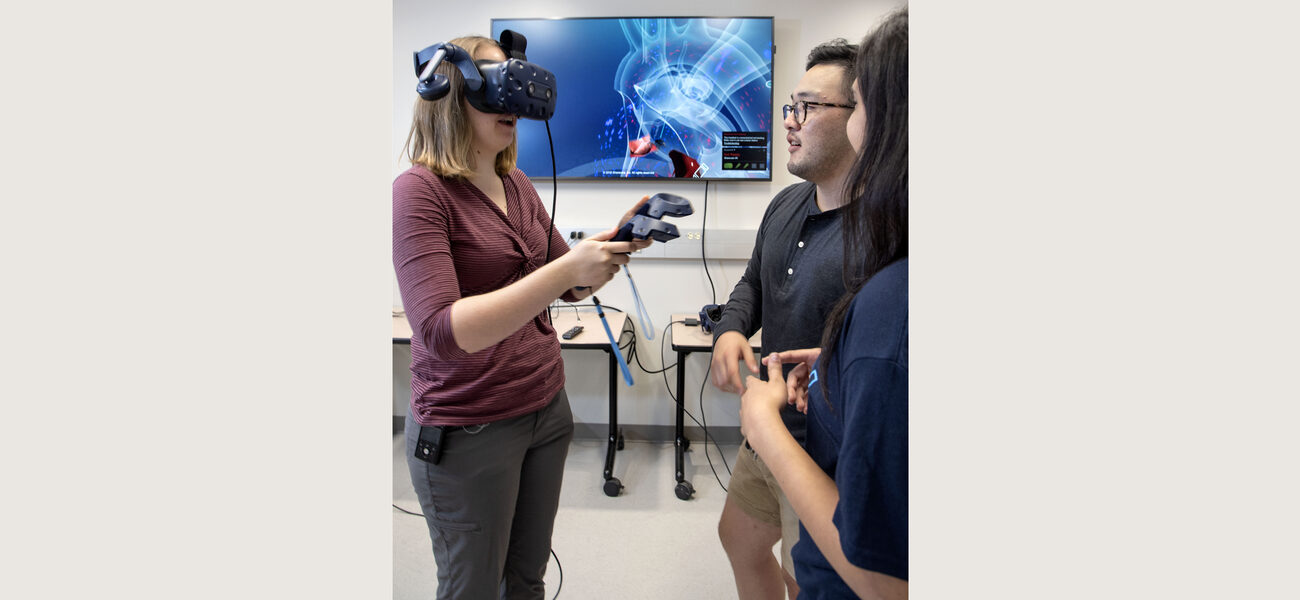
Another important component of the medical school is its use of virtual reality. In the VR suite, students can use headsets to see three-dimensional models of the brain, heart, and other organs, and explore how the various systems operate. Faculty members watch what students are looking at on a large wall monitor.
“From virtual reality to the reality of the simulation lab, discussion and exploration are done non-intrusively. It’s better that mistakes are made in the lab than in real life,” says Liu. “Technology can enhance human decision-making, such as in medicine, but nothing can fully replace field experience, so students will spend time training at the Carle Hospital.”
Bioengineering faculty and their research groups use the first-floor laboratories and collaboration spaces to study such topics as image-guided surgical systems, biomedical nanotechnology, gene editing, regenerative medicine, and gene circuits.
The third floor houses several state-of-the-art BSL-2 instructional labs supporting studies on tissue engineering, bio-fabrication, and genetic engineering.
Students gain knowledge in quantitative biology techniques and gain experience performing bacterial and mammalian cell cultures.
Making laboratories modular was key to the renovation project, according to Larson. Researchers frequently come and go, and changes in staffing are inevitable. Instead of a complete remodel, which is cost prohibitive, benches and other furniture are moveable in all of the instructional and research labs.
Robust wireless technology was also a priority to ensure “zero latencies,” which means no delay.
“Robots are performing a surgery,” says Liu. “Say you are in San Francisco, and the doctor is here to operate a machine to perform a delicate procedure. Or, the command is going to Brazil to perform eye surgery, and that laser is cutting. In the medical field, the data must be current and accurate; latency can mean life or death.”
Students start working in research labs as undergraduates, some in their freshman year. Exposing them to the medical school early in their university experience is advantageous.
“Bio-engineering and medicine have been converging for several years,” says Larson. “If we have those within the same spaces, and if undergrads see both disciplines going on at the same time, engineering students may make the decision to go to medical school.”
Open Collaboration Encouraged
Instructional spaces and common areas are set up so that students can mingle, communicate, and work together. The laboratories themselves also have that open environment.
“Not only does the infrastructure configuration have to support the needs of a fast-changing field, but the open space encourages the user to come in, to interact, and let the ideas flow,” says Liu.
Open space means “a little more than open,” says Larson. “They are cross-disciplinary work areas. You bring in mechanical, electrical engineering, and physics together because it takes all the components and disciplines to create a lot of the things we do in engineering today, especially at the medical level.”
Students can develop designs for certain kinds of medical instruments, make new biometric sensors, and collaborate with other engineering specialties to design soft materials. For example, soft polymers are used in bioprinting cells that can be used for tissue or organ fabrication.
Students also are trained in data analytics. “We’re blending future doctors’ intellectual curiosity with engineering know-how,” says Liu. “Future doctors will be able to search one billion records of back history of patients within a second or two.
“We have engineers with the capability of inventing a microchip in a certain robotic device to deliver a cancer-fighting drug directly to the cell at the nano level,” he continues.
Lui envisions a day when soft materials, jointly developed by engineers and doctors, will be able to do things like repair heart valves or provide fewer side effects for burn patients, using sensors.
“We’re working in that direction,” he says. “The more doctors and engineers know and are trained in each others’ field, the more likely we can come up with those innovative solutions we dream about.”
The curriculum was jointly created by bioengineering and medical faculty, and students receive the benefits of being taught by teachers with different expertise.
“Having mentors from both fields allows students to learn different ways of thinking and triggers their intellectual curiosity,” says Liu. “One is more science-related and the other is more problem-solving, and we integrate those to challenge students and stimulate their creativity and inventiveness. Students get the best of both worlds.”
The medical field is data- and technology-intensive, and the possibility of performing medical testing remotely means that the school is contributing to healthcare not only in the U.S., but world-wide.
“People realized this is the wave of the future of medicine,” says Larson. “We, as a team, brought this building to fruition, and the programs in it are going to change the world.”
By Susan Gonsalves